If you have fibroids it can sometimes feel like you are on a long and tortuous conveyor belt. Symptoms, tests and scans, a diagnosis, and more appointments. Then, finally, when a line of treatment is offered – relief that this long and exhausting process and the difficult symptoms that prompted it, are coming to an end. And the temptation is to just go with the surgery or drug that is being offered. But what do you really need to know about fibroids before you make any decisions?
What Are Fibroids?
Fibroids are benign growths of muscular and fibrous tissue that can occur in the uterine/womb cavity (submucosal), or grow from the uterine wall to the outside of the uterus (subserosal), or grow within the uterine wall itself (intramural). There are also fibroids that can grow on a stalk both in or outside of the uterus and these are called pedunculated fibroids.
Fibroids are Common
Many women can develop fibroids. Around 1 in 3 women developing them at some point in their lives. Unless they cause symptoms a woman may be unaware that she has them. If they are not giving you problems through symptoms, or as a result of their physical location they are not a particular issue, they may not require any treatment.
Do Fibroids Go Away On Their Own?
 Some good news – yes, fibroids usually shrink after menopause! Fibroid growth is thought to be linked to oestrogen. We grow them during our fertile years when our oestrogen levels are at their highest. They start to shrink as you enter your peri-menopause as your natural levels of ovarian oestrogen dip. If you can manage the symptoms naturally then surgery or drugs, with the potential for side effects or long-term issues, might not be needed.
Some good news – yes, fibroids usually shrink after menopause! Fibroid growth is thought to be linked to oestrogen. We grow them during our fertile years when our oestrogen levels are at their highest. They start to shrink as you enter your peri-menopause as your natural levels of ovarian oestrogen dip. If you can manage the symptoms naturally then surgery or drugs, with the potential for side effects or long-term issues, might not be needed.
Fibroids and Cancer
Sometimes women worry that their fibroids may turn into cancer. Thankfully, it is rare for a developing fibroid to be cancerous, and current medical thinking is that it is unlikely that an existing fibroid will become cancerous. And having fibroids does not necessarily increase the risk of developing cancerous fibroids or other forms of cancer in the uterus. But if you are worried it is a good idea to put your mind at rest by talking to your doctor.
Fibroids Symptoms
There may be some women who have no symptoms and no issues from their fibroids. They may never even know they have them. However, for some the symptoms can be really difficult to manage and finding the best way forwards a priority.
These will vary according to your constitution and health, and the type and location of the fibroid(s) you may have. But symptoms of fibroids may include:
- Irregular, heavier or painful periods. This can be debilitating so it is important to address, and to take into account additional measures alongside the fibroid management itself. If you periods are particularly heavy, prolonged or frequent you may need to check you are not becoming anaemic and look at taking an additional iron supplement such as Spatone.
- Back pain or abdominal discomfort – which could be worse during your period.
- Pain or discomfort during sex
- Urinary symptoms – such as need to urinate more often from pressure on the bladder.
- Fullness, bloating or other sensations – in your abdomen from the fibroid itself, you may feel like you have gained weight and if your fibroid is large enough you might have. But it could also be that you have a sensation of fullness and feel bigger.
- Feeling the fibroid(s) – Depending upon the size and location of the fibroid you may even be able to feel it if you gently palpate your abdomen around that area.
There can be other symptoms too depending upon how and where your fibroids are. If you think enough of this list applies to you and you have not already done so, it can be sensible to see your GP for an examination so that the diagnosis can be confirmed and other possibilities ruled out.
Fibroids Treatments
Fibroids Drug Treatment
You may be offered drugs and before you say yes, not yet or no, there are important things to consider.
There are drugs that doctors can and do offer to try to alleviate some of the fibroid symptoms like heavy b leeding and pain in the short term. But they will have potential side effects and will not address the imbalance or issue in the longer run.
leeding and pain in the short term. But they will have potential side effects and will not address the imbalance or issue in the longer run.
Your GP or consultant may also consider drugs that effectively reduce the amount of oestrogen in circulation (GnRH analogues). These can work because the growth of fibroids can be increased by oestrogen, therefore if the levels drop they are likely to reduce in size.
This might be offered as an alternative to surgery or prior to surgery to facilitate their removal. However, these treatments can lead to the woman experiencing menopause-type symptoms so she may exchange one set of health challenges for another. It might also only be a temporary respite from the fibroid symptoms if taken instead of surgery, as once stopped and oestrogen levels rise again, the fibroids could grow back.
Progesterone may also be offered to help with the menstrual symptoms, but this has once again the potential to come with side effects and may not be addressing the cause of the fibroids.
As part of your Fibroids drugs treatment plan, I believe it is vital to ask:
• What does the drug do?
• What are the potential short-term and long-term side-effects?
• What will happen if I do not take them?
• What are my options?
If drug-based or surgical routes are taken, there is still the possibility that if a woman is yet to have her menopause she could re-grow her fibroids. As is so often the case, and not just in this field of health, the root cause needs to be worked with. Unless we address that it is just like weeding your garden by taking only the tops off the weeds. And any gardener will tell you what a flawed strategy that is.
Fibroids Surgery
It may be that surgery being offered? If so it is worth researching the various options available as they each have different strengths and weaknesses, and may be suitable for different types of fibroids.
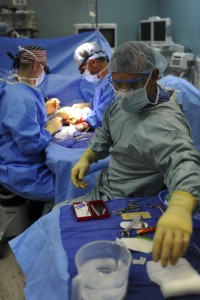 Has the procedure being suggested a track record with a known safety record and efficacy profile? Or is it comparatively new? Many people don’t realise how experimental the field of surgery is. In some ways that can be good as it hopefully moves treatments forwards. But you do need to know to be able to decide how you feel about being part of an experiment as data is gathered.
Has the procedure being suggested a track record with a known safety record and efficacy profile? Or is it comparatively new? Many people don’t realise how experimental the field of surgery is. In some ways that can be good as it hopefully moves treatments forwards. But you do need to know to be able to decide how you feel about being part of an experiment as data is gathered.
As with any procedure it can also be helpful to find a surgeon who is not only experienced in this field but also with the particular procedure in question.
- Fibroids Hysterectomy – full or partial, women are offered this as the way to “solve all the problems”. Whilst this might offer an apparently simple solution to the patient and the surgeon, there are many issues to consider before taking this step. Over the years I have meet a number of women who tell me they wish they had known more before they took this step. You can read more in my blog Hysterectomy Questions to Ask.
There are other procedures that remove the fibroid(s) but leave the uterus in situ:
- Myomectomy – depending upon the woman’s medical history and profile, and the size and location of her fibroids this can be performed where the fibroid(s) is removed in an open procedure (via the abdomen), laparoscopically (through a small incision in the abdomen) or via the vagina.
- Hysteroscopic Resection of Fibroids – this is a procedure that surgically removes the fibroid(s) via the vagina.
- Hysteroscopic Morcellation of Fibroids – this procedure differs from the Resection in that the hysteroscope (telescope) is inserted only once rather than repeatedly. However, this is a relatively new procedure and the NHS website states: “…because hysteroscopic morcellation is a new technique, evidence about its overall safety and long-term effectiveness is limited….”
- A note of caution if you are in The States, and other parts of the world where Laparoscopic Power Morcellators may have been used in the removal of uterine fibroids. The FDA has issued advice against using this technique as it has the potential in some instances to spread undiagnosed cancer cells.
- In the UK the NICE Guidelines for Hysteroscopic Morcellation of Fibroids address some of the differences between the Laparoscopic and Hysteroscopic procedures and also note some issues and complications with the hysteroscopic technique.
- Endometrial Ablation – destroying the womb lining by heat.
- Uterine Artery Embolisation (UAE) – the blood supply to the fibroid is removed and it will therefore stop growing. I must confess to being concerned about the potential for complications as a result of the fibroid tissue breaking down in situ.
- Myolysis – a laser is used on the fibroid. I have similar concerns around this treatment as for the UAE mentioned above.
I would encourage anyone considering any kind of surgical intervention to ask questions of their GP, gynaecologist, homeopath, etc.
Useful questions for women to ask about surgical treatments for fibroids:
• What are my options for helping with the symptoms of the fibroids?
• Have I had an accurate diagnosis – do I need further examinations/scans?
• Do I need further tests/scans to assess the size, location and nature of my fibroids?
• What is my timeframe – how many years before I am likely to have my menopause?
• Can I assess how quickly or slowly they have been growing?
• Are they likely to become much larger and what symptoms might they cause if they do?
• What are the pros, cons, possible complications and success rates of the different surgical options?
• If a hysterectomy is suggested, is it absolutely necessary? If I have one, can I keep my ovaries, fallopian tubes and cervix?
• Are adhesions likely from a surgical procedure and if so, what steps could be taken to reduce them?
• It is also important to note that if a woman is still looking to have children she will need to find out how the fibroids and any treatment options may affect her becoming pregnant, her pregnancy and the birth.
Fibroids Alternative Treatment
It is good to bear in mind who you are talking to, everyone has their bias. Different doctors, surgeons and healthcare practitioners will all have different experience, expertise and preferences in terms of treatments.
Surgeons are attuned intellectually and professionally to perform surgery and to use drugs that support that route. When we wish to discuss our non-surgical options perhaps we ought not to be surprised by an unenthusiastic response.
 Medical doctors will usually suggest taking pharmaceutical drugs and we should not be surprised at their lack of knowledge about non-drug options. The various support group and association websites will each have their particular perspective depending upon how they are set up and their sources of information and funding.
Medical doctors will usually suggest taking pharmaceutical drugs and we should not be surprised at their lack of knowledge about non-drug options. The various support group and association websites will each have their particular perspective depending upon how they are set up and their sources of information and funding.
What is key is that you have the information and support that you need to make an informed decision that is right for you.
Can I Shrink My Fibroids Naturally?
As an alternative health practitioner, this is where my bias shows! I believe you can do a huge amount to help by taking a natural approach. Sometimes there may be reasons why surgery or drugs are a good option. That is when it is so important to ask questions, and to make informed decisions about your treatment. But also taking a natural approach to your self-care before and after any surgery, etc. can support not just your hormonal health, but also your general health. There are good reasons to take care of yourself whatever path you follow.
 I usually work with creating a more hormone-balancing diet like the one I write about in my Foods That Help With Menopause blog. It does not matter if you are not in your peri-menopause as these recommendations can support hormonal balance in general.
I usually work with creating a more hormone-balancing diet like the one I write about in my Foods That Help With Menopause blog. It does not matter if you are not in your peri-menopause as these recommendations can support hormonal balance in general.
We can also tailor homeopathic remedies and herbs to support with some of the specific challenges of having fibroids, and to support a woman’s overall health. It is important too to consider if and how we get a chance to exercise, to relax and to express our creative selves. It is about taking a whole-person approach.
As a practitioner who has specialised in offering women information and support at menopause for over 16 years I have met a lot of women struggling with the symptoms of their fibroids. It is not that it is a menopausal issue as such, just that by the time we get into our 40’s and 50’s we have had a few decades to grow them, and symptoms can often come to a head around this time.
Take a Long-Term View to Solving Fibroid Issues
You are entitled to seek second and third opinions, and onwards until you feel sure that you have been correctly and fully diagnosed because that is critical in determining the best way forwards for you. You need to be fully informed and happy with a course of action both in the short term and the longer run.
For me the most important thing every woman should know about fibroids is that she needs to ask questions. Not to assume that the options presented are the only ones, or the best ones for her. There is more support out there than you might think – get informed, read, and question. It is your body and needs to last you for your lifetime – as happy and as whole as possible.
I hope you have found this post helpful. My practice clinics are in West and East Sussex, and also via Skype. If you would like to consider your options and to see if my approach might suit you, please do contact me.

